Understanding Your Blood Work: What Common Lab Results Really Mean
You’ve just gotten your blood work results back from the doctor. Maybe they’re sitting in a patient portal, a wall of numbers and abbreviations staring back at you. What does it all mean? Is that flagged result something to panic about — or is it perfectly normal for you?
Blood tests are one of the most powerful diagnostic tools in medicine, offering a snapshot of your health that few other tests can match. But understanding what they reveal takes a little context. This guide walks you through the most common panels — what’s being measured, what the numbers mean, and when to have a real conversation with your doctor.
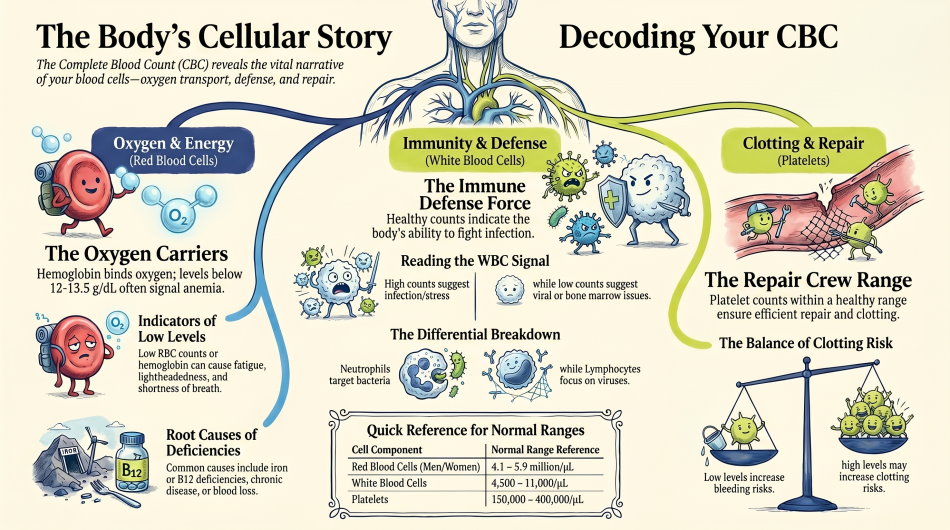
The Complete Blood Count (CBC): Your Body’s Cellular Story
The complete blood count is usually the first test ordered at a routine physical. It measures the three main types of cells circulating in your blood.
Red Blood Cells (RBC), Hemoglobin, and Hematocrit
Red blood cells carry oxygen from your lungs to every tissue in your body. Three numbers describe their health:
- RBC count: The number of red blood cells per microliter of blood. Normal ranges are roughly 4.5–5.9 million/µL for men and 4.1–5.1 million/µL for women.
- Hemoglobin (Hgb): The protein inside red blood cells that actually binds to oxygen. Low hemoglobin — typically below 13.5 g/dL for men and 12.0 g/dL for women — signals anemia.
- Hematocrit (Hct): The percentage of your blood volume made up of red blood cells. This tracks closely with hemoglobin.
If these values are low, you may feel fatigued, short of breath, or lightheaded. Common causes include iron deficiency, vitamin B12 or folate deficiency, chronic disease, or blood loss.
White Blood Cells (WBC)
White blood cells are your immune system’s soldiers. A normal WBC count runs between 4,500–11,000 cells/µL.
- High WBC can indicate infection, inflammation, stress, or — in rare cases — leukemia.
- Low WBC (leukopenia) may suggest a viral infection, autoimmune condition, or bone marrow problem.
Your results may also include a differential, breaking down WBC types: neutrophils (fight bacteria), lymphocytes (fight viruses), monocytes, eosinophils (respond to allergies/parasites), and basophils. Elevated eosinophils, for instance, might suggest allergies or a parasitic infection.
Platelets (PLT)
Platelets are tiny cell fragments that help your blood clot. Normal range: 150,000–400,000/µL.
- Low platelets (thrombocytopenia): Risk of bleeding; can be caused by certain medications, autoimmune disorders, or liver disease.
- High platelets (thrombocytosis): Can increase clotting risk; often a reaction to infection or inflammation.
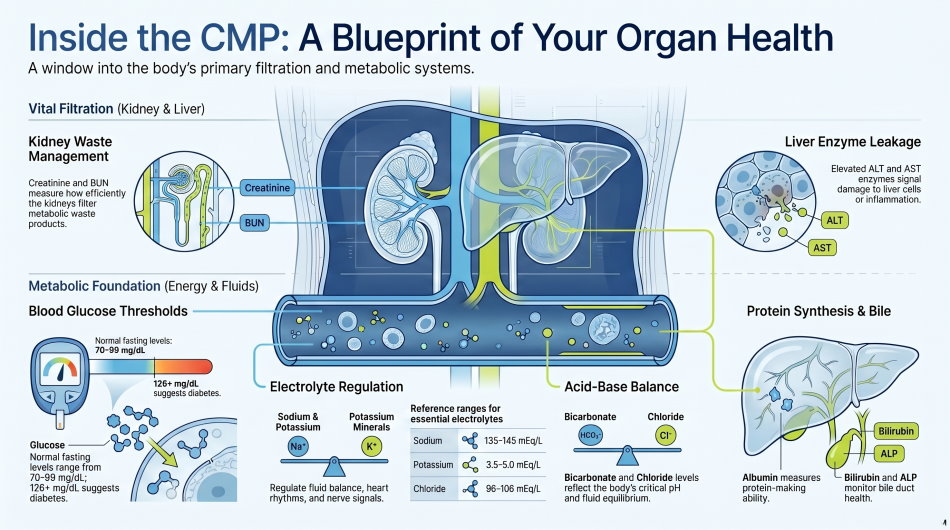
The Comprehensive Metabolic Panel (CMP): Organ Health at a Glance
The comprehensive metabolic panel (or basic metabolic panel, BMP, for a shorter version) checks your blood chemistry — giving your doctor a window into how your kidneys, liver, and metabolism are functioning.
Blood Glucose
Fasting blood glucose measures how much sugar is in your blood after at least 8 hours without eating.
- Normal: 70–99 mg/dL
- Prediabetes: 100–125 mg/dL
- Diabetes: 126 mg/dL or higher on two separate tests
If glucose is flagged, your doctor may also order a hemoglobin A1c (HbA1c) — a 3-month average of blood sugar control — which is more telling than a single snapshot.
Kidney Function: BUN and Creatinine
Two markers tell your doctor how well your kidneys are filtering waste:
- Blood Urea Nitrogen (BUN): A byproduct of protein metabolism. Normal: 7–20 mg/dL. High BUN can point to dehydration, kidney stress, or high protein intake.
- Creatinine: A waste product of muscle metabolism, filtered almost entirely by the kidneys. Normal: roughly 0.6–1.2 mg/dL. Elevated creatinine is a more reliable kidney marker than BUN alone.
Your results may also include eGFR (estimated glomerular filtration rate), calculated from creatinine and age. An eGFR above 60 is generally considered normal; below 60 for three or more months suggests chronic kidney disease.
Electrolytes: Sodium, Potassium, Bicarbonate, Chloride
These minerals regulate fluid balance, nerve signals, and pH. Key values:
- Sodium (135–145 mEq/L): Helps control fluid balance. Low sodium can cause confusion and fatigue; high levels signal dehydration.
- Potassium (3.5–5.0 mEq/L): Critical for heart and muscle function. Both high and low potassium can trigger dangerous heart rhythms.
- Bicarbonate (22–29 mEq/L): Reflects acid-base balance.
- Chloride (96–106 mEq/L): Works closely with sodium.
Liver Function Tests (LFTs)
Several markers assess liver health:
- ALT (alanine aminotransferase) and AST (aspartate aminotransferase): Enzymes released when liver cells are damaged. Elevated levels can point to fatty liver disease, hepatitis, alcohol use, or medication effects.
- Alkaline phosphatase (ALP): Elevated in bile duct problems or bone disorders.
- Total bilirubin: A breakdown product of red blood cells processed by the liver. High bilirubin can cause jaundice and may indicate liver or gallbladder disease.
- Albumin and total protein: Measure the liver’s protein-making ability. Low albumin can signal malnutrition or chronic liver disease.

The Lipid Panel: Understanding Your Cardiovascular Risk
A fasting lipid panel measures the fats in your bloodstream — a key part of assessing heart disease risk.
LDL Cholesterol (“Bad” Cholesterol)
LDL (low-density lipoprotein) deposits cholesterol in artery walls. Lower is generally better:
- Optimal: Below 100 mg/dL (below 70 mg/dL for high-risk individuals)
- Borderline high: 130–159 mg/dL
- High: 160 mg/dL and above
HDL Cholesterol (“Good” Cholesterol)
HDL (high-density lipoprotein) removes cholesterol from arteries. Higher is better:
- Protective: 60 mg/dL and above
- Low (risk factor): Below 40 mg/dL for men, below 50 mg/dL for women
Triglycerides
Triglycerides are fats linked to diet, alcohol use, and metabolic health:
- Normal: Below 150 mg/dL
- Borderline high: 150–199 mg/dL
- High: 200–499 mg/dL
High triglycerides combined with low HDL and high LDL form a pattern often associated with metabolic syndrome and increased cardiovascular risk.
Total Cholesterol
Total cholesterol (ideally below 200 mg/dL) is useful, but context matters enormously. Someone with low HDL and high LDL might have a “normal” total cholesterol but still carry significant risk. Your doctor looks at the full picture, not just one number.
Thyroid Function: TSH and Beyond
The thyroid gland regulates metabolism, energy, mood, and much more. The key screening test is TSH (thyroid-stimulating hormone).
- Normal TSH: 0.4–4.0 mIU/L (ranges vary slightly by lab)
- High TSH: The pituitary is working hard to stimulate an underactive thyroid (hypothyroidism) — symptoms include fatigue, weight gain, and cold intolerance.
- Low TSH: The pituitary is pulling back because the thyroid is overactive (hyperthyroidism) — symptoms include weight loss, anxiety, and rapid heartbeat.
If TSH is abnormal, your doctor may order Free T4 and Free T3 to get a clearer picture of thyroid hormone levels.
A Word on “Normal” Ranges — and Why Context Is Everything
Here’s something most people don’t realize: lab reference ranges are statistical estimates, not hard boundaries between healthy and sick. They’re typically set to capture 95% of a healthy population — which means 5% of perfectly healthy people will fall outside the range on any given test.
A result slightly outside normal might mean nothing for you specifically — or it might be meaningful in the context of your symptoms, history, and trends over time. A single mildly elevated liver enzyme in an otherwise healthy person looks very different from the same value in someone with chronic fatigue and weight loss.
What to do when something is flagged:
- Ask your doctor what the flag likely means given your specific situation.
- Find out whether it needs to be repeated or monitored.
- Ask what lifestyle factors — diet, exercise, sleep, medications — may have influenced the result.
- Don’t diagnose yourself based on a single out-of-range value.
F.A.Q.
There isn’t just one—CBC, BMP, and lipid panels are all essential.
They can be helpful but should not replace professional evaluation.
Yes, stress can impact hormone and glucose levels.
Some tests require fasting; follow your doctor’s instructions.
It doesn’t always indicate disease—further testing may be needed.
10 Proven Best Solutions for Acne That Really Work
Jimenez2026-05-30T04:31:02+00:00May 20, 2026|Categories: acne|Tags: acne trteatments, wellness exam|
Best Solutions for Acne By Sole Health Medical Center Acne is one of the most common skin [...]
Detect Hidden Health Issues Before They Become Serious
Jimenez2026-05-04T23:09:32+00:00March 12, 2026|Categories: physical exams, Prevention|Tags: wellness exam|
🩺 How Primary Care Providers Detect Hidden Health Issues Before They Become Serious Primary Care Providers Detect [...]
Understanding Your Blood Work
Jimenez2026-04-27T20:34:35+00:00February 19, 2026|Categories: physical exams, Prevention|Tags: wellness exam|
Understanding Your Blood Work: What Common Lab Results Really Mean By Sole Health Medical Center You've just [...]
How Primary Care Providers Detect Hidden Health Issues Before They Become Serious
Jimenez2026-04-02T19:37:39+00:00January 15, 2026|Categories: physical exams, Prevention|Tags: wellness exam|
How Primary Care Providers Detect Hidden Health Issues Before They Become Serious” – 7 Powerful Early Warning [...]